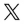Free knowledge to monitor the world of events. Have a look at our must read Blogs on Pharma, Finance, HR, Health and Cross Industry.
The Effects Of Changing Restrictions On Pediatric Drug Development
2022-07-25
Children should receive medications that are customized for them. Over the past few decades, there has been a growing awareness of the necessity of involving children in the drug development process.
In both the EU and the US, legal and regulatory systems are well-established. More research is being done today on pediatric medications than there was ten years ago. All phases of the pediatric drug development pipeline have shown proof-of-concept. It's time to look at how the process of creating medicines for kids has changed within these parameters and decide how this work should be used more broadly. The creation of pediatric medications is discussed in this overview, along with a critical evaluation of the work that has been done within those parameters.
The scientific basis for developing pediatric drugs
Multiple errors were made initially when planning pediatric medication development trials, as can be expected in any new scientific field. For instance, the FDA review division can request a pediatric study that was deemed insufficient for pediatric labeling when it was carried out by the sponsor. In other instances, the medicine dosage was off. 42 percent of all BPCA studies carried out between 1998 and 2012 were not given any pediatric labeling. 7 This was a startling number because all of these medications had been shown to be successful in adults, and there was ethical concern because these failed experiments had not benefited the protected pediatric patient population.
Dosing, the placebo effect in pediatric patients, changes in the illness process between pediatric patients and adults, and research design were important issues in the "failed" (failed to label) trials, according to another examination of those trials. 8 Numerous approaches have been used to address the dosage issue in the development of pediatric medications. Improved pediatric dosing during drug development has resulted from the use of dose range, greater modeling and simulation approaches, and combined adolescent and adult trials. One strategy to combat the placebo effect has been to conduct trials for migraine headaches using a double randomization, which removes placebo responders.
Pediatric Drugs: Opportunities and Challenges
There are still significantly fewer licensed pediatric medication treatments available for children than there are for adults. To enhance and safeguard children's health, international regulatory agencies have given the creation of age-appropriate pediatric dosage forms a higher priority throughout the previous 15 to 20 years. The development of new pediatric pharmaceuticals has seen a major increase in industry research as a result of a mix of unmet patient demands, regulatory incentives, and potential penalties.
When creating a pediatric dosage form, there are a lot of crucial considerations to keep in mind, and the specifications can be very different from those for medication intended for adult usage. Developmental scientists must take into account the child's age, weight, physiological condition, and overall treatment plan in addition to the method of administration, safety profile, general flavor, and palatability. To successfully design a pediatric product that succeeds in the clinical, regulatory, and commercial spheres, it is imperative that all of these crucial factors are properly balanced. However, it might be argued that the biggest issue facing the sector is still the lack of direction and clarity regarding how these development goals can be fulfilled.

-
Utilizing Modeling and Simulation in the Development of Pediatric Drugs
Because children are such a delicate population, it has historically been difficult to develop medications for pediatrics. It is critical to comprehend the subtleties unique to the sector when creating medications for children. Drug developers may confront challenges that can influence whether a clinical trial with children is successful or unsuccessful. These challenges include obtaining informed consent from families, dealing with potential opposition from the children involved, and gaining acceptance from study staff.
The right study designs, knowledge of the various ways that pharmacokinetics (PK) and pharmacodynamics (PD) might vary in children, early involvement with regulatory agencies, and use of the proper modeling and simulation methodologies are other essential elements that must be present for success.
Regulatory Advice for pediatrics’ Study Plans
With the addition of new legal requirements by regulatory agencies like the US Food and Medication Administration (FDA) and the European Medicines Agency, pediatric drug research has been more and more encouraged and controlled throughout time (EMA). The majority of medication development programs only have one shot to be successful in identifying a safe and effective dose level because pediatric clinical investigations continue to be challenging. The requirement that the dose range encompass all pediatric age groups, including neonates (newborn infants), adolescents (12–16 years old), and all ages in between, adds to the complexity.
The FDA offers a pediatric research design and extrapolation algorithm in the draft guideline encompassing general clinical pharmacology concerns for pediatric studies for medicines and biological products. This decision tree from a pediatric trial aids in deciding when extrapolation is appropriate for efficacy and when it is not. When efficacy may be extrapolated, at the very least, a PK study and a safety trial will be necessary (which can occasionally be merged into a single experiment). If extrapolation cannot be done, a dose-ranging study followed by a further pediatric safety and efficacy trial will be anticipated.
Modeling Methods Crucial to Pediatric Development
The development of pediatric medications has benefited greatly from developments in PK/PD modeling and simulation tools, which promote the best trial designs. Drug developers can increase the number of participants and length of a trial, reduce the burden of sampling for PK, biomarkers, and/or endpoints, and do a lot more by using model-informed drug development (MIDD) methodologies. The following are some significant modeling and simulation methodologies for the development of pediatric medications:
- Population PK analysis
- Allometric scaling and extrapolation
- Simulations of clinical trials
Conclusion
Over the past ten years, pediatric medication development has advanced significantly. Trial failure rates in pediatric studies, which once approached 40%, are currently under 20%. Although the future appears incredibly bright, new pressures are starting to build. There are still outstanding problems regarding the proper use of extrapolating adult efficacy to pediatric patients as well as the use of modeling and simulation to reduce or do away with pediatric clinical trials.
Given our improved knowledge of pediatric disorders and the development of pediatric drugs, the failure rate for pediatric research should be 10% or less. However, history has proven that pediatric doctors are tenacious and committed, so in the future, these inquiries will have their answers for the good of young patients.
Do you want to understand more about Pediatric Drug Development ? Join us at the Pediatric Drug Development MasterClass on 05th to 07th September, 2022.
By Rajeethan Thaventhiran, SEO & IT Executive, GLC Europe, Colombo Office, Sri Lanka.
Get a feel for our events

Training Program for CMC Leaders - EU edition
14th September 2026 - 09th April 2027
Rich with practical insights and real-world applications
learn more >>
Training Program for CMC Leaders - US edition
14th September 2026 - 09th April 2027
Rich with practical insights and real-world applications
learn more >>
Real World Smart Packaging & ePILL Solutions for Pharma MasterClass - US edition
26-27 May 2026
Evolution and progression of smart packaging
learn more >>